How a new innovation will share vital information when a person with dementia is in hospital
The hospital journey tracker makes it easier to support a relative or friend with dementia in hospital.
Her mother had Lewy body dementia, frontotemporal dementia and hearing loss. She also couldn’t speak English and didn’t trust many people.
Tiziana Groom couldn’t have been clearer when she talked to the hospital – she needed to discuss her mother’s discharge and be at her side to help her when it took place.
This didn’t happen. The nurses had been told by a different department to prepare her mother for leaving hospital.
‘They dressed Mum, put on her hat and sat her in a wheelchair,’ says Tiziana, her full-time carer who had lasting power of attorney.
‘She thought she was going home. Then they called me and said, “Your mum is ready to go.” I asked, “Go where?” and was told she was going to a care home.
‘I hadn’t agreed this. No one had spoken to me. So they undressed her and helped her back into bed.
‘Of course, Mum became frustrated, confused and extremely distressed. She was stuck in hospital for another two unnecessary weeks.
‘I kept trying to get hold of the right person who had the authority to discharge Mum, appropriately, with a care plan.’

Tiziana and her late mum.
This was just one of many miscommunications that led Tiziana to join a focus group looking at smoothing the process of leaving hospital.
Tiziana’s feedback helped Alzheimer’s Society, working with hospitals in Bedfordshire and software company Phew!, to develop a way of enabling people to keep track of what’s happening and what will happen next when a relative or friend with dementia is in hospital.
Named contacts
The hospital journey tracker emails named contacts, updating them on a person’s treatments and plans for discharge. This means someone’s contact is better able to support them, ensuring their discharge is safe and not delayed unnecessarily.
The pilot schemes, including one at Luton and Dunstable Hospital, have had an excellent response, with many saying they felt more involved in discharge planning and better prepared for leaving hospital.
In the words of David, who lives with dementia, ‘Something like this could revolutionise how people get out of hospital.’
Matthew Burgess, Managing Director at Phew!, describes the balancing act of not creating too many additional demands on busy healthcare teams by asking them to fill in details on the tracker, while still providing useful information for carers and family members.
‘We’re looking for minimum impact on the staff and maximum support for the patient and their families,’ he says.
He adds that, when his grandmother was in hospital with dementia, none of his family had much sense of what was happening to her. He understands how needed this service is.
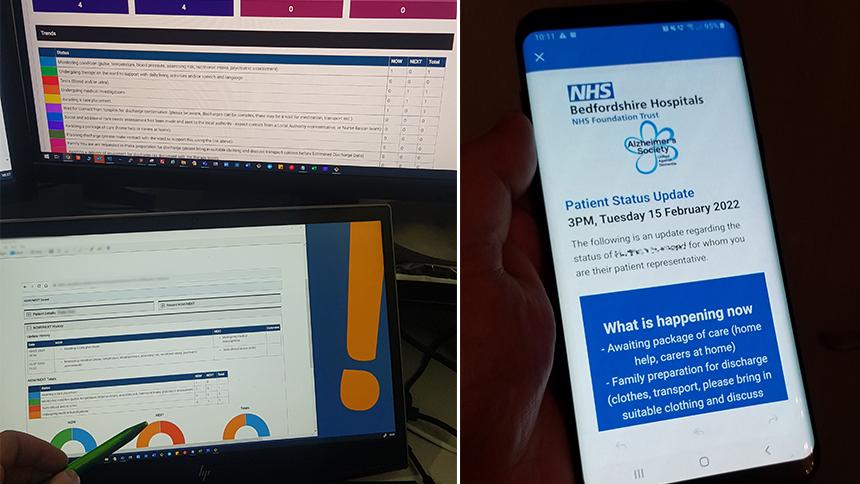
Eased minds
The tracker sends information about the treatment the patient is undergoing and what will happen next.
‘It’s so much better than calling and hoping to speak to a doctor,’ says one of those involved in the pilot, while another adds, ‘This has eased my mind and given us a definite date of discharge.’
Ella Moonan-Howard, Alzheimer’s Society’s Senior Innovator, explains that the tracker was developed with the help of people with personal experience of hospital admissions, as well as health and social care professionals.
‘We know there are many different challenges concerning hospital discharge for people with dementia who’ve been deemed medically fit but stay in hospital longer than needed,’ she says.
‘This is partly down to issues with communication. It’s difficult for any patient or carer to absorb the information that they’re being given by busy staff and relay that to others. These challenges are exacerbated when a patient has cognitive difficulties, because they’re less able to relay that information themselves.
‘When hospital staff are going on their ward rounds with our tracker, they can tick if someone has dementia and updates will automatically be sent to the patient’s representative.
‘Being in hospital is always an anxious experience. We want to be able to reassure people that their loved one is being discharged from hospital into the right environment and that they know what support is out there.’

Matthew and Ella.
Further development
The system is now being developed further with Phew! to find ways to make it more personalised, and to allow it to share information with more contacts.
‘We’re expanding the tracker to find ways to support people to feel empowered and make choices,’ explains Ella. ‘We want them to play an active part in preparing someone for discharge.
‘Our ideal is to help feedback the likes and dislikes of the patient, so they can be cared for in the best possible way.
‘Carers have an intimate understanding of individuals with dementia. They need to be able to share this knowledge.’
Help develop the tracker
Do you have a recent hospital discharge experience to share?
Contact [email protected] before 28 February 2023 to help develop the tracker further.

