Missing freedom: Cherishing every moment with Mum
After a year’s separation from his mum, the return of face-to-face care home visits means the world to Jamie Greaves.
‘I was in full PPE and met by someone in a hazmat suit – it was like a science fiction film,’ says Jamie Greaves, recalling his first ‘window visit’ to his mum’s care home during the pandemic.
‘She recognised me but became hysterical and wanted to climb out, so had to be restrained by staff. It was actually quite horrendous.’
Like so many carers, friends and relatives, Jamie has found it incredibly upsetting to be denied proper visits to a loved one with dementia.
‘My mum is my world, she brings a great deal of joy to my life,’ he says. ‘I felt so guilty to suddenly stop visiting.’
With visits still restricted, Jamie continues to call for change.
‘I want it to go back to an open-door policy. Care home residents aren’t prisoners,’ he says.

Patricia brings a great deal of joy to Jamie’s life.
Starring role
Jamie’s mum Patricia, now 73, spent much of her working life as a secretary or PA for managing directors of large companies. She later moved into bookkeeping and her own CV-writing business. She was also involved with local singing and drama groups.
‘She was always taking the starring role!’ says Jamie, a freelance creative consultant who lives in Brighton. ‘She was very lively, social and active.’
Jamie is an only child who was born after Patricia had already experienced a series of miscarriages, and the pair have always been close.
‘There wouldn’t be a day without some sort of contact,’ he says.
Sketchy diagnosis
Patricia always loved the sunshine and around 10 years ago moved to Tenerife with her partner. Some years later, it started to become clear that something wasn’t right with her health.
‘She would repeat herself in emails, or phone me twice in three minutes, not realising we’d already spoken,’ says Jamie. ‘Her friends said she came back from a restaurant and got plates out to start cooking a meal.’
After what Jamie describes as a ‘sketchy’ diagnosis of Alzheimer’s disease in Tenerife, Patricia and her partner moved back to the UK to live in Stoke-on-Trent, to get a proper diagnosis and further support. But having struggled to come to terms with how dementia was affecting Patricia’s behaviour, her partner walked out.
‘It was devastating for Mum – she just kept asking where he was,’ says Jamie.

Jamie says his mum used to be very social and active.
Completely hysterical
Jamie got social services involved, who said that Patricia needed to go to a dementia assessment unit.
‘That was one of the hardest things I’ve ever done,’ says Jamie. ‘I was told to get Mum chatting to staff and then edge out through a side door. It was very upsetting, although also a relief to get her properly assessed.’
A later visit from Jamie proved distressing for both of them.
‘Mum freaked out and was completely hysterical,’ he says. ‘She was kicking out at staff and screaming at me that I’d put her there and didn’t love her. I broke down in tears, which was when she snapped out of it and calmed down.’
Patricia was ‘sectioned’ – detained under the Mental Health Act. She spent 10 weeks on a hospital psychiatric ward, where she was diagnosed in December 2018 with frontotemporal dementia (FTD) and bipolar disorder.
FTD is a less common type of dementia that can cause changes to a person’s personality and behaviour, and difficulties with language. Bipolar disorder is a mental health condition that can cause someone’s mood to swing from one extreme to the other.

Patricia’s move to a home near Brighton meant Jamie saw her most days.
Caged lion
Patricia went to live in a specialist nursing home in Stoke for people with dementia, with Jamie visiting every weekend from Brighton. However, Patricia would become very upset when he wasn’t around, so in mid-2019 Jamie moved her to a home near him.
‘I was there most days and would take her out on the seafront or to the shops or pub,’ he says. ‘I would do her nails and hair – she loved that. There were still some separation issues but overall it worked really well.’
Then came the pandemic, and Jamie was no longer allowed to be with his mum.
‘I was devastated,’ he says. ‘She couldn’t understand about the pandemic or that I wasn’t allowed to visit, so it was a horrendous time and very upsetting.
‘I lost many nights’ sleep thinking about it, and as it went on the frustration built and built.’
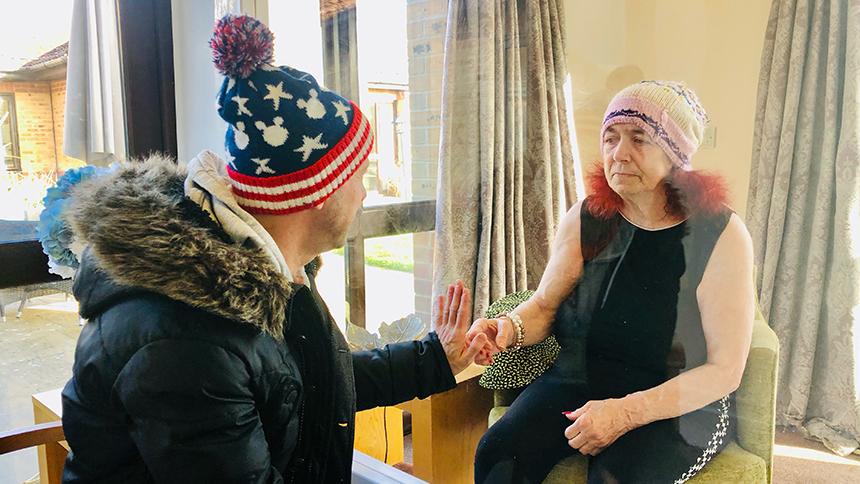
Patricia found video calls confusing and window visits distressing, while pod visits were also unsuccessful.
‘She was behind a pane of glass but wouldn’t settle,’ says Jamie. ‘She was like a caged lion, trying to find a way out to be where I was.’
Although Jamie found the home’s manager to be understanding, in his opinion, care home companies have tended to be overly cautious.
‘I think that people’s deterioration during lockdown has been worse than the risk of COVID in some respects,’ he says.
Jamie helped to raise awareness of the importance of proper visits on social media, writing to his MP and also sharing his experiences in support of an Alzheimer’s Society campaign.
‘I think there was a period where the government weren’t fully understanding the magnitude of the situation,’ he says.
Future risk
Jamie’s grandmother also had dementia, and that prompted him to try a self-testing DNA kit.
The Society doesn’t recommend these kits, because they aren’t as reliable as tests done by the NHS and it can be easy to misunderstand what the results mean without personalised advice from a professional.
However, Jamie’s test said he had a slightly increased chance of developing Alzheimer’s and he adds, ‘It does make me think about the future.’
Being a single gay man with no children or siblings has an impact on what this would mean too.
‘I don’t see much visibility of support for LGBTQ people with dementia or their family members and partners.
‘It would be nice to see care homes catering specifically for this demographic, especially as gay people may be more likely to be left without a partner or family to care for them.’
Cherished moments
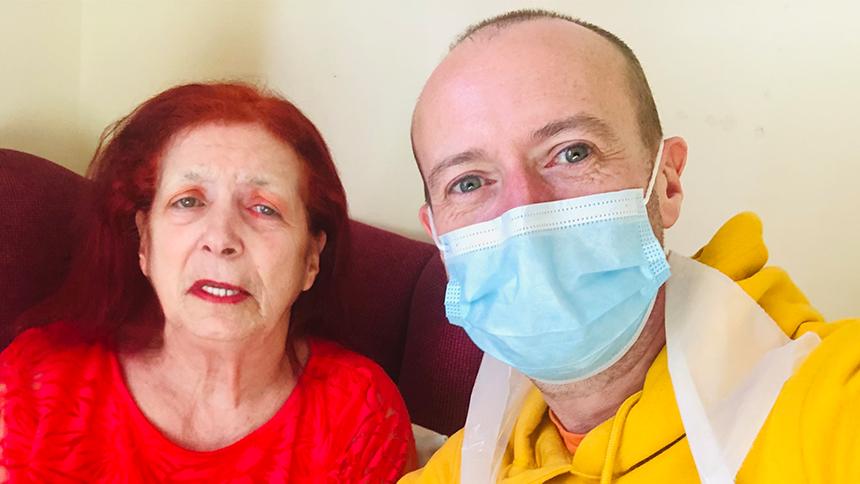
Jamie can now visit his mum once a week if he takes a COVID test beforehand and wears PPE.
‘It’s still not ideal, but it’s noticeably better,’ he says.
‘It seems odd to say, but after the year we’ve had, even being able to visit for 30 minutes meant the world. Seeing her face light up is worth a million dollars to me.’
Patricia has had both doses of the COVID vaccine and Jamie is now waiting for the frequency and flexibility of pre-pandemic visits to return.
‘I miss that freedom of longer visits. Mum gets quite sleepy now and sometimes struggles to talk, so when she’s animated and chatty I want to make the most of it,’ he says.
And as Jamie reflects on a ‘horrendous’ year, the importance and value of his visits are as great as ever.
‘You’ve got to cherish moments with the people that you love, because you don’t know how dramatically things can change from one moment to the next.’
What can you do to help?
You can help ensure that more carers like Jamie receive the support that they need.


Pam
saysI so agree with Jamie in all that he has said and only wish the powers to be would have listened much much earlier, maybe even understood that keeping them from their family’s was and is the wrong thing to do.
My Mum is 91 and has Alzheimers she has been in a care home now for 3 years, before the pandemic I would visit her most days and we would chat and do a bit of knitting, reading or jigsaw puzzle. Then due to the pandemic I stopped coming we tried through the window, FaceTime, phone none were successful, then they built what I can only say was a very very small cell and called it a visiting pod, knowing my Mum she would be terrified so never used it.
I was so glad when we could start visiting again but oh what a difference in my Mum she did not speak much let alone do any kind of activity, it would take me the full 30 mins visiting time to get her to respond to me and I found it all very upsetting.
Fortunately the manager of the care is amazing and really understands the residents needs with her help I have now become an essential care giver and visit as often as I can staying as long as is required. All I can say is it’s wonderful but it should not be like this we should not be fighting to see our loved ones it’s all so wrong.
Wishing Jamie all the best.
Sherry
saysMy mother passed 7 weeks ago today. She spent the last year under covid lockdown in long term care. I will never get over it. We put her in long term care. 5 days later, lock down. For 4 months, no visits. By the time we saw her, omg. Finally I was allowed in as a designated care giver. She almost passed away last October. They finally allowed the family in, only because she was dying. She pulled through and for the next 6 months I was able to get into her room, have lunch with her. Couldn't take her out due to covid19. God gave me 6 more months. She told us she tried to stay alive but was tired. No pain like dying with vascular dementia.
Sherry, we're really sorry to hear this – it sounds like you have been going through such a difficult time.
Please know that we are here to provide you with support. You can speak with one of our Dementia Advisers by calling our Dementia Connect support line on 0333 150 3456. Find more information about the support line, including opening times, here: https://www.alzheimers.org.uk/dementia-connect-support-line
Cruse Bereavement Care also have a helpline and resources that may be of interest: https://www.cruse.org.uk/
You might also like to talk with other people affected by dementia within our online community, Talking Point. Feel free to browse and read others' experiences, or you can create an account to reply and connect with others who may have been through a similar situation: https://forum.alzheimers.org.uk/
Please do call the support line on 0333 150 3456 when you need someone to talk to, Sherry. You are not alone.
Alzheimer's Society website team
Susan Hope
saysDear Jamie
I also live in brighton and my mother is now a resident in a nursing home in
Ditchling
She to suffers from Alzheimer’s and is end stage
I completely heard and felt every word of your recollections of lockdown and Covid —19 and how it had impacted in such. Cruel and horrendous way on our loved ones.
Nobody should be treated like our elderly relatives have been
It has been a travesty and utter flagrant violation of their human rights
They have been treated like prisoners in what is supposed to be classed as their own home
The scars run deep and the hurt and pain indescribable
I too like you Jamie can not wait for open visits to come and go as we please and spend long periods with the pe we love so much
I will continue to campaign until this becomes reality
Finally my mother has just suffered at the hands of the local CCG who have decided to take her CHC funding away after 15 months despite still having primary health needs !!!
So I now have a long battle in my hand s to fight for her and prove her entitlement
I wish you and your mother lots of good wishes and continue with your campaign
Christine OBrien
saysI feel so sad for Jamie having to deal with his Mum having Dementia at such a young age and he must certainly find out about becoming an Essential Care Giver giving him more frequent access..
My Mum has Alzheimers and has been in a Nursing Home for 6 months but she is 92 and has had a very interesting life.. My sister and I are privileged to still have her in our lives..
Nichola Lines
saysOutrageous that there is no balance of needs between the awful Covid-19 threat (via individual risk assessments) and severe mental health needs.. I currently have two very sick parents age 87 & 90 with dementia/Alzheimer’s and other complex issues including stroke. My father can no longer speak, and is at high risk of aspiration/choking to death. I’ve just been told I can only see him for “half an hour” per week only. He has been to date been used to seeing me daily, he had previously relied upon my mother for care until she could no longer do it. My mother who got out of a “prison-like” NHS mental health hospital ward (they should know better) where she was being assessed for her Alzheimer’s disease, and other complex needs, worsening as she now has extreme depression too, went in able to walk and now can barely shuffle forward. Seeing her panic at being locked in a room yet again, with me this time able to see through the double glazed high up window was horrendous for me and yet more hours of unimaginable anxiety for her. She has not committed a crime, she just wants to be near her husband who she has only ever been separated from when my brother and I were born and her som and daughter. Today I visited the local NNUH care trust hospital and the COVID risk signed clearly signed is “low”. (I was allowed in here daily). On her first day locked in her new care home amongst total strangers alone in her room she accidentally shut herself in the bathroom and couldn’t get out. I heard her desperate calls for help. I couldn’t get in to help, nor could I telephone the home as I had no phone signal. I finally alerted someone by knocking on an adjacent bedroom window. There is no common sense in rulings that are interpreted differently by every care home and hospital. One hospital with150 people with dementia some end of life and extreme allows essential carers in daily, another mental health hospital only one hour per week. The law (or rather “guidelines” are an “ass” they say, people and families of the most sick and vulnerable who have no voice literally in my father’s case or one that’s not heard (in my mother’s case) are being completely ignored. If the Alzheimer’s Organisation & John’s Campaign and the friends and families of this large number of people in society cannot be heard, how is my lone voice to my MP going to change this horrific situation. Another Hillsborough? The worst death toll from COVID-19? This is not a political issue, this is a human rights issue.
Alzheimer's Society
saysHi Nichola,
Thanks for your comment. We're really sorry to hear about your parents - it sounds like you have been going through a very difficult time.
Please know that you can always call our Dementia Connect support line on 0333 150 3456 for more information, advice, and support specific to your family's situation. More details about the support line (including opening hours) are available here: https://www.alzheimers.org.uk/dementia-connect-support-line
You might also like to talk with other people affected by dementia within our online community, Talking Point. This could be a great place for you to share experiences and receive helpful suggestions from other people who have been in similar situations: https://www.alzheimers.org.uk/get-support/dementia-talking-point-our-on…
We hope this is helpful, Nichola,
Alzheimer's Society blog team
Lovelyn Umeloh
saysThank you Jamie for the love of your mum. The sadness and joy of this story is very emotional and I hope things get better to enable you have more time with your mum. Why not since it makes both of you feel good,
Caroline
saysHow sad that Jamie is feeling lucky to be granted just 30minutes once a week. Since he clearly makes such a wonderful difference to his mum's well being, and gets her out and about, it's disappointing that he hasn't been granted Essential Care Giver status so he could visit daily if wished.
I hope things continue to improve for Jamie + his lovely mum, and for all other families who continue to be cruelly and unnecessarily separated xx